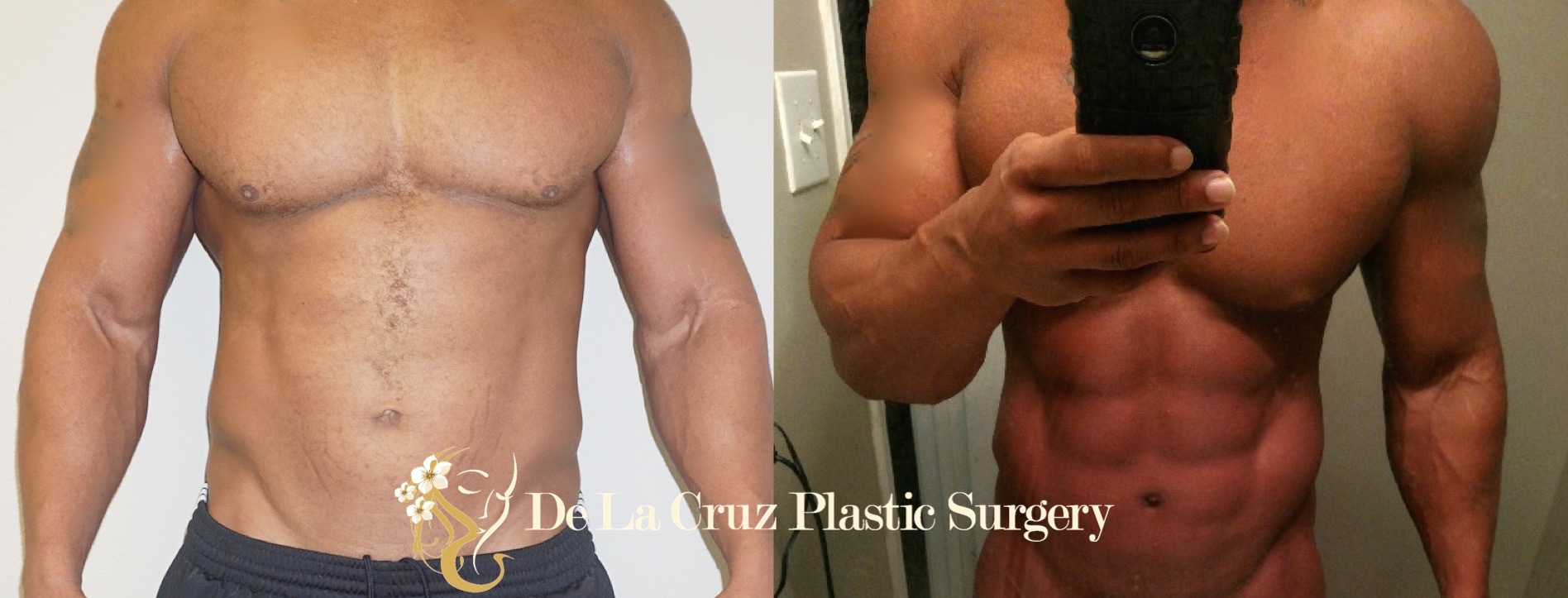
VASER Liposuction: A Good Source for Mesenchymal Stromal Cells
Mesenchymal stromal cells (MSCs) are the spindle shaped plastic-adherent cells isolated from bone marrow, adipose, and other tissue sources, with multipotent differentiation capacity in vitro. These mesenchymal stromal cells could differentiate to bone in vitro and a subset of the cells that has a high proliferative potential . The notion of a mesenchymal stem cell was popularized by Arnold Caplan proposing that MSCs gave rise to bone, cartilage, tendon, ligament, marrow stroma, adipocytes, dermis, muscle and connective tissue. Adipose-derived mesenchymal stromal cells (ASCs) are concentrated in fat tissue, and the ease of harvest via liposuction makes them a particularly interesting cell source. Thus, fat has been transferred to the face for facial rejuvenation, as well as to the buttock for buttock augmentation. It has shown that radiation-induced damage skin are dramatically improved by fat transfer.
Recently, ultrasound-assisted liposuction using VASER liposuction and Lysosonix were found to harvest viable mesenchymal stromal cells. "UAL samples demonstrated equivalent ASC yield and viability. VASER Liposuction adipose-derived mesenchymal stem cells showed higher osteogenic and adipogenic marker expression, but a comparable differentiation capacity was observed. Soft tissue healing and neovascularization were significantly enhanced via both UAL-derived ASCs in vivo, and there was no significant difference between the cell therapy groups."
VASER Liposuction allows safe and efficient harvesting of the mesenchymal stromal cellular fraction of adipose tissue and that cells harvested via this approach are suitable for cell therapy and tissue engineering applications.
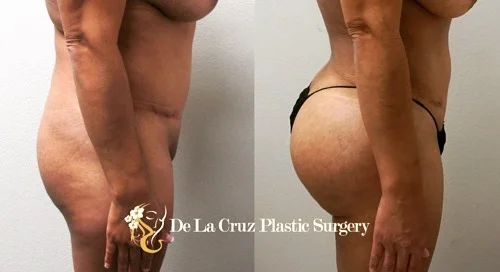
Recent studies have shown that adipose tissue derived using the VASER liposuction system were viable at harvest and suitable for autologous fat grafts, such as in Brazilian Butt Lifts. The study had shown that "the lipolysis assay revealed metabolically active adipocytes with a mean (SD) correlative viability of 85.1%. Direct measures of acute viability via propidium iodide staining resulted in a mean (SD) viability measure of 88.7%.
Reference:
Duscher, et al. Ultrasound-assisted liposuction provides a source for functional adipose-derived stromal cells. Cytotherapy. 2017 Sep 13. pii: S1465-3249(17)30658-8. doi: 10.1016/j.jcyt.2017.07.013. [Epub ahead of print]
Schafer et al. Acute adipocyte viability after third-generation ultrasound-assisted liposuction. Aesthetic Surgery Journal. 2013 Jul;33(5):698-704. doi: 10.1177/1090820X13485239. Epub 2013 May 29.
Emmanuel De La Cruz MD, PLLC